Prolapse
- Home
- /
- Prolapse
Prolapse
Uterine prolapse occurs when the uterus descends from its normal position into or beyond the vaginal canal due to weakened pelvic floor muscles and ligaments. It can range from mild (where the uterus drops slightly) to severe (where it protrudes outside the vagina). This condition can cause discomfort, urinary or bowel issues, and can significantly affect a woman’s daily life.
Uterine prolapse is most common in postmenopausal women who have had multiple vaginal deliveries, but it can affect younger women too.
Causes and Risk Factors
Pregnancy and childbirth (especially multiple or complicated deliveries)
Aging and menopause (drop in estrogen weakens pelvic tissues)
Chronic coughing or constipation
Heavy lifting or strenuous physical work
Obesity
Previous pelvic surgery
Genetic predisposition to weak connective tissue
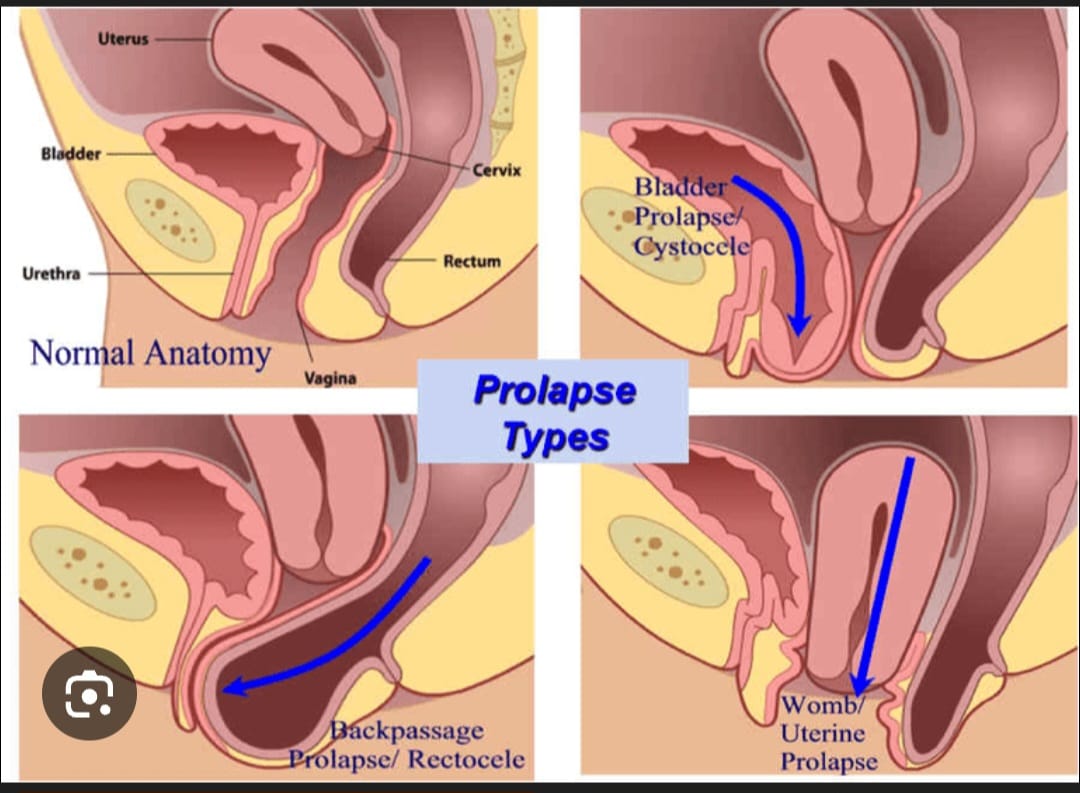
Symptoms of Uterine Prolapse
Symptoms may vary depending on the degree of prolapse and can include:
A feeling of heaviness or pressure in the pelvis
Bulge or protrusion from the vaginal opening
Urinary incontinence or difficulty urinating
Frequent urinary tract infections
Difficulty with bowel movements
Lower back pain
Pain or discomfort during intercourse
Sensation of something “falling out” from the vagina
Grades of Prolapse
First-degree: Uterus drops slightly into the vagina
Second-degree: Uterus descends close to the vaginal opening
Third-degree: Uterus protrudes from the vagina
Fourth-degree (Procidentia): Complete uterine prolapse, with the entire uterus outside the vaginal canal
Treatment Options for Uterine Prolapse
Pelvic floor physiotherapy (Kegel exercises) to strengthen support muscles
Pessary device: A silicone ring inserted into the vagina to support the uterus (ideal for those avoiding surgery)
Hormonal therapy: Estrogen creams in postmenopausal women to strengthen tissue
Uterine Suspension: Repositioning and anchoring the uterus using native tissue or mesh (uterus-preserving)
Vaginal Hysterectomy: Removal of the prolapsed uterus via the vaginal route
Laparoscopic/Robotic Uterine Suspension or Hysterectomy: Minimally invasive methods with faster recovery and minimal scarring
Repair of associated prolapse: Such as cystocele or rectocele repair (if needed)
Advantages of Minimally Invasive Surgery
Less post-operative pain
Shorter hospital stay
Quicker recovery
Minimal visible scarring
High success rates with long-term relief
Why Choose Dr. Kalpana Tiwari for Prolapse Treatment?
With more than 15 years of surgical expertise in minimally invasive and reconstructive gynecology, Dr. Kalpana Tiwari offers advanced, patient-tailored solutions for uterine prolapse. Her strengths include:
Expertise in robotic and laparoscopic prolapse repair
Uterus-preserving procedures for younger patients
Gentle, respectful care for elderly or postmenopausal women
Collaborative approach to restore comfort, dignity, and quality of life


